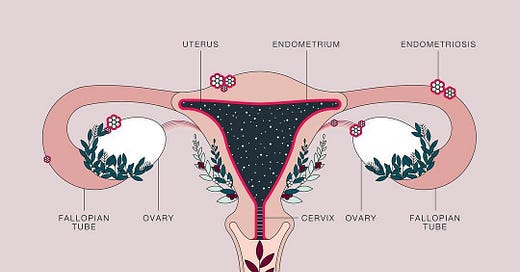
Hey friends! I couldn’t let the month of March — aka endometriosis awareness month(!) — go by without re-sharing this goodie. This was originally published in 2022, when I had about half the readership that I do now. If you’re new since then, I’m so glad you’re here! If you’re a hardcore oldie, you’re a goddamned rock star. Thank you!
Later this week, I…
Keep reading with a 7-day free trial
Subscribe to Adventures in vaginas (and other parts) to keep reading this post and get 7 days of free access to the full post archives.