Hey friends! I’ve got a lot of fun announcements re: book club, my new course, and more, so please make sure you scroll to the bottom to get those!
Lastly, if you’re a monthly subscriber, be sure to scroll to the end to get some goodies!
Lately, I have been on a journey. A poop journey.
I’m kind of obsessed with poop — my poop, my kids’ poop, and my clients’ poops.
Sorry, TMI? Since you’re already here, I didn’t think so. I’ve been on the struggle bus with my gut, hormones, and general autoimmune issues this last year, and constipation has reared its ugly head.
But I haven’t turned to laxatives. Here’s why I think it’s worth fighting for the real deal when it comes to pooping.
Here’s the tl;dr:
There is a time and a place for everything. You NEED to be pooping on the regular, so if laxatives are your only choice, use them with no judgement.
Constipation is multifactorial. I will be covering the main and most common offenders here, but there is so much that is highly individualized — the state of your gut flora, your sex hormone status, etc.
You do not have a laxative deficiency, and laxatives are not meant to be used on a long term basis. If you need laxatives to poop/make it happen on the regular, work with a professional to figure out what is driving your dysfunction and to create a plan to live laxative free.
My raison d’etre for writing this is that constipation totally fucks up your pelvic floor for about a million reasons. It worsens stress and urge urinary incontinence, prolapse symptoms, pelvic pain, fecal incontinence — I could go on, but I did in this article, so read more there.
The deep dive:
Are you, in fact, constipated? There are many different definitions of functional constipation, but here’s my definition of “ideal”. Anything less than this is… you guessed it, constipation!
You should be pooping 1-3x/day, pain free and easy
Your poop should look like a number 3 or 4 on the Bristol Stool Scale (see chart below)
You should feel a sense of complete emptying — not like you have more in there!
Here’s that gorgeous chart, for reference:
It should be noted that a lot of people (and kids!) experience what’s called overflow constipation, which typically looks like diarrhea. This is because the bowel is so blocked up that only mushy stuff can get around the proverbial boulders in the tube (sorry, I know it’s gross).
A typical pattern with this is to begin the day with a slightly more firm or even constipated bowel movement, and then have multiple additional poops that progressively looser as time goes on. A lot of these folks struggle with skid marks and full blown fecal incontinence, and are shocked to discover that the driver of the problem is constipation. I’m telling you — it is!
So now we know who’s constipated and who isn’t. If you’re constipated, read on.
You need to be pooping, and pooping well. I cover the why behind this crusade in this gem of an oldie. Suffice to say, it matters a lot when it comes to how your pelvic floor functions and thrives (or doesn’t).
But! It. Is. Not. Okay. To. Depend. On. Laxatives. To. Poop. Regularly.
Exceptions: Absolutely use laxatives (whatever is recommended by your provider) for one to two weeks after giving birth, especially if you had a c-section. Similarly, any surgery warrants a course of laxatives, as opioids in anesthesia are a known driver of some gnarly constipation. Specific medical conditions, like spinal cord injuries, also warrant consistent use of laxatives and enemas, but that’s a different conversation entirely.
Finally, as I have previously stated, you absolutely need to poop. If you are not pooping and in pain or discomfort, for goodness sake, use a freaking laxative. It’s fine. You’re a good person! Just don’t think about it as a long term plan.
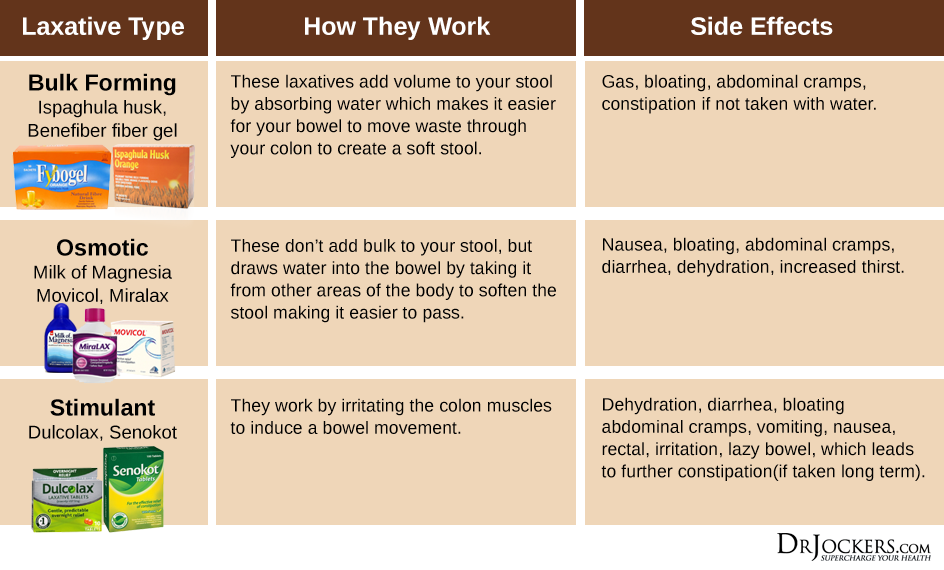
Okay, let’s start with some basics. Here’s a cute little chart of the different types of laxatives and their mechanisms:
So why are laxatives a less than ideal plan? I’ll address my qualms by category:
Bulk Forming: I actually don’t have a huge issue with these, other than the fact that many brands contain lots of fillers and dyes that aren’t great for your long term GI health. If you know extra fiber helps your poop, and you’re unable to get those sources through your diet, then this is totally fine. Depending on if you have a FODMAP sensitivity issue, you might do well with psyllium, acacia fiber, or PHGG (partially hydrolyzed guar gum), which is a prebiotic. It’s worth playing around here. In many academic papers, fiber supplementation isn’t even considered a laxative, so there.
Osmotics: This is a controversial but important one — maybe the most important? The big issue here is the primary ingredient in Miralax, polyethylene glycol (PEG) 3350. There is LOTS of controversy around PEG in general, but the big one is that it causes neuropsychological side effects, like tics, OCD-type behaviors, aggression, etc. While these are case reports, there have been enough complaints that have been acknowledged by bodies like the Neurogastroenterology and Motility Committee and in one paper, 16% of pediatric gastroenterologists reported that patients complained of such adverse reactions.
Furthermore, osmotics and particularly PEG 3350 have been recently associated with gut permeability and motility changes, which leads to shifts in the microbiome and nutrient absorption. This [horrifying] paper demonstrated an association between long term use of laxatives and dementia incidence. This is certainly not showing causation, but it’s enough to take pause, I think.
It should be noted that PEG 3350 is not FDA approved for use in children, and it is only recommended for a seven day use span in adults. While it is generally considered safe, there is also a lack of robust data.
Stimulants: The challenge with stimulants is pretty straightforward: your body gets used to them, and then becomes dependent on external laxative stimulants to trigger peristalsis of the bowel, i.e. what moves everything along.
Here’s the take-home:
I know that a lot of y’all are potentially freaking out by now. Let’s take a deep breath!
You’re a good person. I’ve said that already, but I’ll just keep saying it.
Let me repeat that there is a time and a place for everything. Also, while I have brushed on the topic of kids + constipation, that’s really a whole other newsletter. Let me know if you want me to write about it, because I have things to say!
So let’s talk about how to make magic happen in the bathroom.
The first thing to assess is what is driving your constipation. Could it be your pelvic floor (see this article for more info)? If so, see a pelvic floor therapist! If you truly think that’s not the case, here are some big, low-hanging fruit:
Nervous system dysregulation: There, I said it. Ever heard of the parasympathetic nervous system being called the “rest and digest” state? Yeah. About that. When you’re stressed the fuck out, the physical nerves in your gut don’t fire to support digestion. This is a huge contributor to constipation and wildly unaddressed.
Water intake: Pretty self-explanatory. There are many thoughts on this, but a general rule of thumb is to try to get half of your body weight in ounces. (E.g. if I weight 160 lb, I try to drink 80 oz of water/day.)
Fiber: This is tricky, but also real. How much? What kind? VERY bio-individual. Fiber is not a panacea, but it is a real deficit in most folks’ diets. It’s worth exploring increasing natural dietary sources and supplementation, and working with a nutritionist as appropriate for support.
Lack of movement: Your body needs movement input to digest appropriately. This is also a massively overlooked driver of constipation, and it’s worth taking seriously. You don’t need to be an athlete, but you do need to move (probably more than you think). While I am at it, I loved this book on that very subject!
Remember, these are the bare basics. There is SO much more that could be contributing; thyroid issues, pelvic floor tension (I’ll just keep saying it), autoimmune issues, environmental factors, etc.
I will also go on record to say that I think magnesium supplementation, which is technically an osmotic, is totally fine/usually great. About half of the US population is deficient in magnesium, and the adverse side effects are minimal. I personally use magnesium citrate and am all about it.
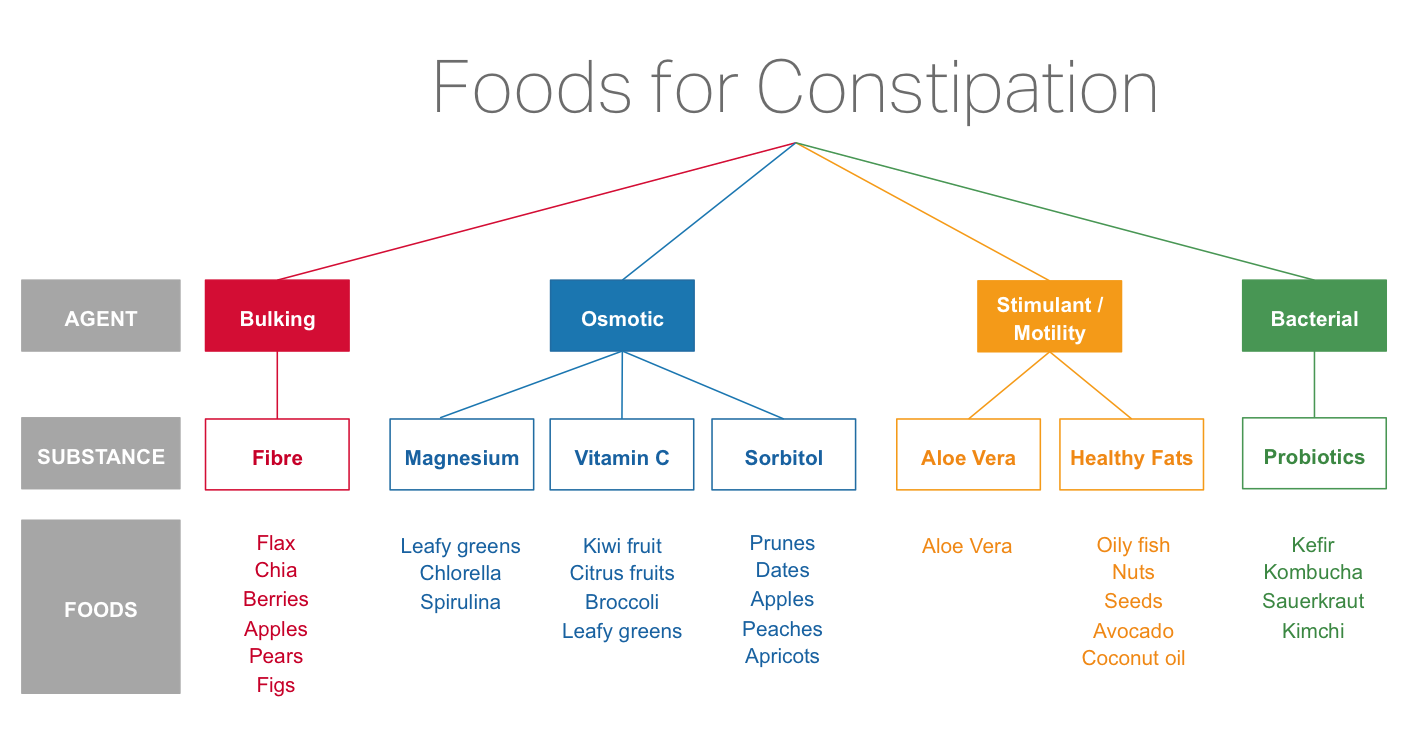
If you want to continue to experiment with food-based interventions, I loved this helpful graphic that breaks it all down:
Hang in there, friends. Remember that you are a rock star, you’re doing a knock-up job, and these things often take a long time and a lot of support to sort out. Keep at it — you’re worth it!
If you’re a monthly subscriber, this is your cue to scroll all the way to the end for a PDF of my hella effective morning routine that puts your bowels on a system and gets you pooping! If you want to be a monthly subscriber and support my work, here’s your cue!
Announcements!!
My course, The Pain Free Pelvis, is launching tomorrow, this coming Tuesday! Think of this course as a little toe in the water for working with me, combining breath work and movement and wrapped in a cute little coaching framework bow so that you can make it accessible to your life. If you are a monthly subscriber, you get the early bird price ($67 instead of $87!). You’ll receive an email with info the day it drops, so subscribe now!
Book club this month will be discussed a podcast series, The Retrievals! While I LOVE this series and think it evokes so many important conversations, it is not for everyone, and if you’re currently undergoing fertility treatment or have fertility trauma, I do not recommend it. We will be meeting on Thursday, October 26, at 8 pm EST, and everyone is welcome. Last time was such a freaking delight and I can’t wait to do it again! See the link in the tab on the home site.
I continue to take rolling applications for coaching clients. If you are looking for support for chronic pelvic pain, I’d love to work together. Find the application here.
I’m so pleased to share my tried and true, universally applicable, bowel routine!