Heeeyyyyyyyyy again!
Greetings, once again, from the UK. I’m having a blast here; feeling the general joys of functional public transportation and the presence of a nationalized health care system (although yes, I know it’s got its issues).
While I’ve been here, I met up with a friend who is hoping to have her second kid soon. It made me thing of allllll the things that are so commonly unaddressed in pregnancy care in the US.
When I was pregnant, I was told that pubic symphysis dysfunction, commonly known as lightning crotch and referred to here as SPD, is an annoying norm of pregnancy, and would go away with birth.
That’s bullshit. Let’s talk about why.
(PS — before I get into it, I have lots of fun announcements re book club, courses, etc— please scroll to the. end so you can be a part of the fun!)
Here’s the tl;dr:
SPD is a very common condition that arises during pregnancy. It can persist into the postpartum period, and rarely affect folks of any gender at any time in life.
It’s not called lightning crotch for nothing — SPD can feel like a literal bolt of pain, sometimes centered in the pubic bone, and sometimes traveling down one or both inner thighs. Fun!
Common advice given by providers is to not do anything asymmetric, and this simply doesn’t make sense. Let’s do better.
The deep dive:
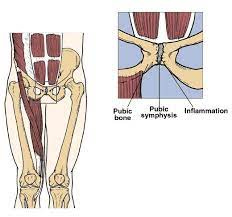
SPD is a condition that feels nearly ubiquitous in pregnancy, but in reality affects about 32% of pregnant folks. The pubic symphysis, aka the place in between the two pubic bones in the front of the pelvis, is part of a larger ring of the pelvis (shocking, I know!) and therefore can be a part of a greater constellation of pelvic girdle pain, including low back pain, sacroiliac pain and dysfunction, and generalized soreness/shitty feelings.
Let’s consult our friend, anatomy, to see the connection!
It’s important to note that pelvic girdle pain, which includes pubic symphysis related pain, occurs in about 45% of pregnant folks and 25% of postpartum folks. SPD can persist postpartum — up to 25% of those who experience it during pregnancy may also get the joy of a postpartum lightning crotch situation, complete with a new human to care for and any additional birth injuries, emotional or physical.
One in four is a lot, and a huge reason why I bristle at the whole “just have the baby and you’ll feel better” schtick.
Some hallmark symptoms of SPD include (but are not limited to!):
sharp, persistent pain in the pubic bone area
sharp pain running down one or both legs
pain with walking, wide legged stances, anything asymmetrical, and rolling in bed
Cool, right? Really fun. It is important for me to distinguish between pubic symphyseal widening, which can cause agonizing pain, and true pubic symphysis separation, which is rare, and causes even more truly exquisite, agonizing pain. When I refer to SPD here, I am referring to what is considered the very common phenomenon of symphyseal widening, not a true separation, which has no consensus on best treatments.
If you suspect you may have a true separation, particularly if you are still experiencing pain postpartum, push for imaging and comprehensive care. Do not accept a shoulder shrug from any provider.
In wild times kinda news, we don’t know exactly what causes SPD, or any pregnancy-related pelvic girdle pain (PPP) in general. Here are a few evidence-based theories:
muscle weakness
carrying multiples (love you, kids, thanks)
biomechanical strains of the pelvic girdle ligaments and associated hyperlordosis (“over-arching”) of the lumbar spine
hormonal shifts leading to ligamentous laxity, a.k.a. blame relaxin
increased neonatal weight (aka weight of the baby) — which interestingly and importantly does not correlate to maternal weight gain during pregnancy.
Critically, additional key factors influencing the incidence and severity of PPP are stress levels and job satisfaction. This finding means that, like all other pain, we need to take a biopsychosocial approach to management and treatment.
This leads me to a tiny rant on treatment strategies. When I was training to be a pelvic floor therapist, here’s what I learned about treating SPD: release the adductors (inner thigh muscles) and teach the client to limit asymmetrical movement as much as possible, giving them “safer” alternatives.
This. Does. Not. Make. Sense.
You know what is asymmetrical? Walking. Also asymmetrical? Stairs. Really fucking asymmetrical? Walking up stairs whilst carrying your toddler or pet or latest Amazon delivery. It is not reasonable to limit this kind of movement, and furthermore, it’s disempowering.
Research tells us that fear-based avoidance behaviors around movement and associated catastrophic beliefs are correlated to increased pain perception. Why, in the good hell then, are we telling pregnant people to make their movement worlds smaller by avoiding basic tasks of living? Why wouldn’t we empower folks to feel safe in their bodies by strengthening the muscles attaching to the pubic symphysis and pelvic girdle and establishing balance among them?
Okay, my rant is over.
Here’s the take-home:
Not to give away the farm or anything, but stabilizing exercises work.
I personally ascribe to the myofascial sling theory, which purports that the anterior oblique sling (i.e. the obliques and adductors) support the pubic symphysis. (Check out this great blog for more.)
When treating folks with SPD, I emphasize using the opposite side oblique and adductor, while additionally firing the transverse abdominis and gluteus medius, who are also star players in overall pelvic stabilization.
Additionally, it’s important to take a function-oriented, movement-first approach. Yes, there very well could be “trigger points” of muscle tension in the adductors, lower rectus abdominis (six pack muscle), pelvic floor or obliques that contribute to pain, and releasing them will definitely help you feel better.
But. You want to walk, right? Carry your kid or object of choice up the stairs?
Let’s do exercises that meet you where you are but build up to these activities in a safe and sequential way.
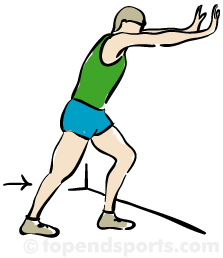
One of my favorite, go-to exercises is a warrior 1 against the wall. I spoke about this exercise in my accessible strength newsletter, and it just so happens to be one of my faves for SPD. Here’s how to do it:
Stand in a lunge (see above) while facing a wall with your arms extended and hands on the wall. If you’re in a lot of pain, begin with your feet hip width apart (no lunge) and simply press into the wall, feeling your deep core naturally respond by engaging. Feeling safe and okay? Amazing! Then, take one foot back into a baby, tiny, not even a real lunge-lunge.
Squeeze your feet towards one another and push into the wall. This action should isometrically activates your adductors (inner thigh muscles) and the front glute medius (that “side pocket” glute), while. the pushing against the wall will continue to get your deep abdominals on board. If this painful, or you don’t feel that side pocket glute in the front leg, try pressing down through the inner heel of your front foot and only squeeze the legs together with 50% effort. Slowly increase the length of your lunge over time.
Then, press down on that front heel to get the glute going and step your back foot forward. Do the other side.
Oh shit, we’re mimicking walking! You can progress this by placing a blocks under your front foot and another one next to it, hip width apart. This mimics stairs.
BOOM!
There are a few other gems I love as go-to’s for SPD. If you’d like some videos, paid subscribers can scroll to the end to get a little bundle of goodies.
Most importantly, know that you are not screwed. Getting your deep core on board with basic movements can dramatically reduce your experience of pain experience, and create a positive feedback loop of less pain » less fear and movement avoidance » even less pain.
A simple hack is to begin an exhale before you roll in bed or the moment before you stand up from sitting. While there’s often more to it, I’ve seen this work wonders.
You’ve got this. Seek care and support, because you deserve to be in less (dare I say no!?) pain. I am, as always, rooting for you.
Paid subscribers: scroll to the end for your videos!
Announcements!
Our book club is this coming Thursday, October 26, at 8 pm EST! We will be discussing a podcast this time (fancy!) — The Retrievals. Trigger warning: this content centers on fertility abuse and trauma. It is fantastic, but be tender with yourself when deciding whether or not this is for you.
My new course, The Pain Free Pelvis, is live! This is a great way to dip your toe in the water if you’re interested in coaching with me, or want to address pelvic pain in an accessible, nervous system-centered way.
If you’re interested in going deep, I am currently taking applications for pelvic pain coaching! Access the application here or email me directly at cait@ritualpelvichealth.com.
Lastly, I’ve created substack threads so we can chat more! I’m a little lonely there, so please come hang. This newsletter was inspired by someone in the chat, so it’s a great way to be heard.
Let’s get you some relief!
Below are my go-to favorite exercises for supporting folks with SPD. Hang in there, friend!
Keep reading with a 7-day free trial
Subscribe to Adventures in vaginas (and other parts) to keep reading this post and get 7 days of free access to the full post archives.





![Pelvis: Anatomy [+ Labeled Diagram] | Concise Medical Knowledge Pelvis: Anatomy [+ Labeled Diagram] | Concise Medical Knowledge](https://substackcdn.com/image/fetch/$s_!6UrM!,w_1456,c_limit,f_auto,q_auto:good,fl_progressive:steep/https%3A%2F%2Fsubstack-post-media.s3.amazonaws.com%2Fpublic%2Fimages%2Fd1d731bd-fa7c-47d1-8910-78b6b0fd1d48_2320x1546.jpeg)